When someone’s blood flow or breathing stops, seconds count. Permanent brain damage or death can happen quickly. If you know how to perform cardiopulmonary resuscitation (CPR), you could save a life.
Cardiopulmonary resuscitation (CPR) is a lifesaving technique useful in many emergencies, including a heart attack or near drowning, in which someone’s breathing or heartbeat has stopped. Although rescue breathing techniques were used to revive drowning victims as early as the 18th century, it wasn’t until 1960 that external cardiac massage was proven to be an effective revival technique.
The American Heart Association recommends that everyone — untrained bystanders and medical personnel alike — begin CPR with chest compressions.
Here’s advice from the American Heart Association:
- If you’re not trained in CPR, then provide hands-only CPR. That means uninterrupted chest compressions of 100 to 120 a minute until paramedics arrive. You don’t need to try rescue breathing.
- Trained but rusty. If you have previously received CPR training but you’re not confident in your abilities, then just do chest compressions at a rate of 100 to 120 a minute.
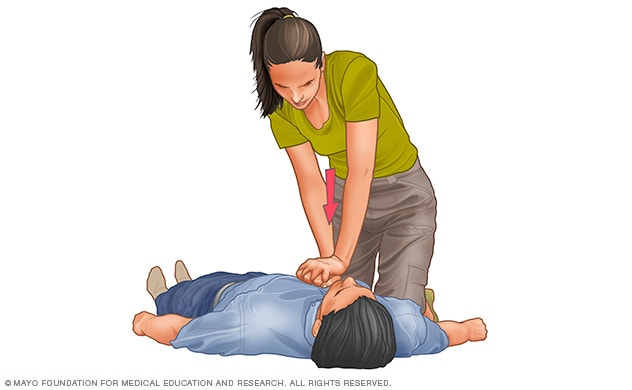
- Trained and ready to go. If you’re well-trained and confident in your ability, check to see if there is a pulse and breathing. If there is no breathing or a pulse within 10 seconds, begin chest compressions. Start CPR with 30 chest compressions before giving two rescue breaths.
The above advice applies to adults, children and infants needing CPR, but not newborns (infants up to 4 weeks old). CPR can keep oxygenated blood flowing to the brain and other vital organs until more definitive medical treatment can restore a normal heart rhythm.
When the heart stops, the lack of oxygenated blood can cause brain damage in only a few minutes. A person may die within eight to 10 minutes.
By performing CPR, you circulate the blood so it can provide oxygen to the body, and the brain and other organs stay alive while you wait for the ambulance. There is usually enough oxygen still in the blood to keep the brain and other organs alive for several minutes, but it is not circulating unless someone does CPR. CPR does not guarantee that the person will survive, but it does give that person a chance when otherwise there would have been none.
If you are not sure whether a person is in cardiac arrest or not, you should start CPR. If a person does not require CPR, they will probably respond to your attempts. By performing CPR, you are unlikely to cause any harm to the person if they are not actually in cardiac arrest.
CPR is most successful when administered as quickly as possible. It should only be performed when a person shows no signs of life or when they are:
- Unconscious
- Unresponsive
- Not breathing or not breathing normally (in cardiac arrest, some people will take occasional gasping breaths – they still need CPR at this point. Don’t wait until they are not breathing at all).
The basic steps for performing CPR can be used for adults, children and infants. They are based on guidelines updated in 2010 that are easy to follow and remember. This information is only a guide and not a substitute for attending a CPR course. The basic steps are:
- D – Dangers?
Check for dangers. Consider why the person appears to be in trouble – is there gas present or have they been electrocuted? Might they be drunk or drug-affected and consequently a hazard to you? Approach with care and do not put yourself in danger. If the person is in a hazardous area (such as on a road), it is okay to move them as gently as possible to protect both your and their safety.
- R – Response?
Look for a response. Is the victim conscious? Gently shake them and shout at them, as if you are trying to wake them up. If there is no response, get help.
- S – Send for help
- A – Open airway
Check the airway. It is reasonable to gently roll the person on their back if you need to. Gently tilt their head back, open their mouth and look inside. If fluid and foreign matter is present, gently roll them onto their side. Tilt their head back, open their mouth and very quickly remove any foreign matter (for example, chewing gum, false teeth, vomit). It is important not to spend much time doing this, as performing CPR is the priority. Chest compressions can help to push foreign material back out of the upper airway.
- B – Normal breathing
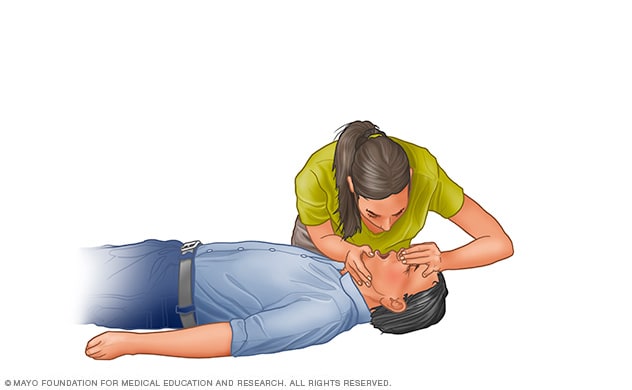
Check for breathing – look, listen and feel for signs of breathing. If the person is breathing normally, roll them onto their side. If they are not breathing, or not breathing normally, go to step 6. The person in cardiac arrest may make occasional grunting or snoring attempts to breathe and this is not normal breathing. If unsure of whether a person is breathing normally, start CPR as per step six.
- C – Start CPR
- D – Attach defibrillator (AED).
CPR may revive the person before the ambulance arrives. If they do revive:
- Review the person’s condition if signs of life return (coughing, movement or normal breathing). If the person is breathing on their own, stop CPR and place them on their side with their head tilted back.
- If the person is not breathing, continue full CPR until the ambulance arrives.
- Be ready to recommence CPR if the person stops breathing or becomes unresponsive or unconscious again. Stay by their side until medical help arrives. Talk reassuringly to them.
It is important not to interrupt chest compressions or stop CPR prematurely to check for signs of life – if in doubt, continue full CPR until help arrives. It is unlikely you will do harm if you give chest compressions to someone with a beating heart. Regular recovery (pulse) checks are not recommended as they may interrupt chest compressions and delay resuscitation.
Learn more about CPR in the video below:
Reference: